TriWest: Definition, Coverage, Application, Benefits, Alternatives

TriWest Healthcare Alliance administers healthcare benefits for veterans and eligible beneficiaries under the U.S. Department of Veterans Affairs (VA) and TRICARE programs. According to the National Institute for Health Care Management (2020), TriWest works with local healthcare providers to deliver essential medical and mental health services to veterans in regions where VA facilities are not available.
TriWest offers a wide range of healthcare services, including medical treatments, mental health care, therapies, and prescription medications. It coordinates with community providers to ensure veterans have access to necessary treatments like substance abuse programs and psychiatric care.
Eligibility for TriWest includes veterans enrolled in the VA healthcare system, active-duty service members, National Guard and Reserve members, and their families.
Key benefits of TriWest are access to a large network of healthcare providers, specialized support for veterans, and comprehensive coverage for various medical and mental health services.
Alternatives to TriWest include TRICARE, the Veterans Affairs (VA) Health Care System, and private health insurance plans.
What Is Triwest?
TriWest Healthcare Alliance is a healthcare provider that administers health benefits for veterans, military families, and other eligible beneficiaries under the U.S. Department of Veterans Affairs (VA) and the TRICARE program.
It provides access to healthcare services by coordinating with local providers, ensuring that veterans receive the care they need through a network of healthcare facilities. TriWest manages the VA’s Community Care Network, offering various services such as medical and mental health, as well as preventive care.
The company partners with the VA to give veterans more options and shorter wait times for services. TriWest operates in areas where the VA healthcare system does not provide the necessary treatment in-house, allowing beneficiaries to receive care from local providers under the VA’s guidelines.
According to a 2020 report by the National Institute for Health Care Management, approximately 10% of U.S. veterans rely on the VA for healthcare, with a growing demand for community-based care programs like TriWest to reduce wait times and improve access.
Did you know most health insurance plans cover mental health treatment? Check your coverage online now.
What Does Triwest Cover?
TriWest covers mental health support, therapies, and medications. TriWest coordinates care with local healthcare providers, ensuring that veterans can access the services they need in their communities.

The treatments Triwest covers include:
- Addiction Treatment: TriWest covers programs for substance abuse treatment, including inpatient and outpatient rehabilitation services.
- Mental Health Issues: TriWest provides coverage for mental health services, including therapy, counseling, and psychiatric care.
- Therapies: TriWest covers various therapeutic services, such as physical therapy, occupational therapy, and mental health therapies.
- Medications: TriWest offers coverage for prescription medications related to the treatment of addiction, mental health disorders, and other health conditions.
What Mental Health Treatments Are Covered by Triwest?
The mental health treatments covered by TriWest include intensive outpatient programs, partial hospitalization programs, and ongoing recovery support, ensuring comprehensive care for those struggling with their mental health. They are designed to support veterans in overcoming mental health challenges through both inpatient and outpatient programs.
The mental health treatments covered by Triwest are as follows:
- Partial Hospitalization Program (PHP): PHP is a step-down program from inpatient treatment that offers a high level of care but allows patients to return home at night. This program includes daily treatment sessions such as therapy, counseling, and medical monitoring, helping patients transition back to their daily lives. It is suitable for individuals who no longer require 24/7 inpatient care but still need intensive support for their mental health.
- Intensive Outpatient Program (IOP): IOP provides flexible treatment for individuals who can live at home but need structured treatment for their mental health disorder. It includes group therapy, individual counseling, family therapy, and psychiatry support, with 3-5 sessions per week. This program is ideal for patients who have made progress in their recovery, but need ongoing support to keep their momentum..
- Outpatient Mental Health Treatment: Outpatient treatment allows individuals to receive care while living at home and continuing with their daily activities. This treatment includes individual counseling, group therapy, and support services, on a less intensive schedule than IOP. It is suitable for individuals with mild to moderate symptoms who need flexible, ongoing support.
What Therapies Are Covered by TriWest?
The therapies covered by TriWest include Cognitive Behavioral Therapy (CBT), Dialectical Behavior Therapy (DBT), Individual Therapy, and Group Therapy. These therapies are designed to address both the psychological and emotional aspects of mental health disorders, helping individuals develop coping strategies and build healthier behaviors.
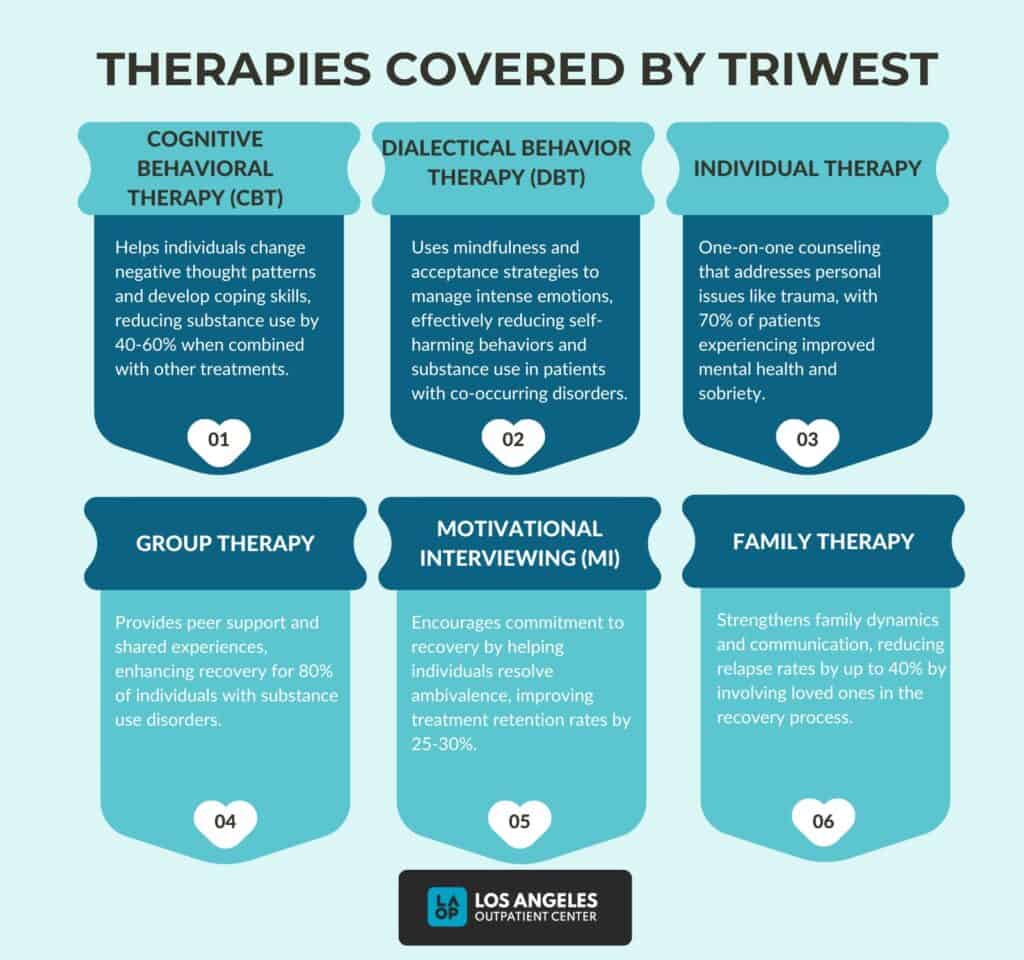
Common therapies covered by TriWest include:
- Cognitive Behavioral Therapy (CBT): CBT helps individuals identify and change negative thought patterns and behaviors associated with mental health disorders. It equips patients with coping skills to manage triggers and stress, improving emotional regulation.
- Dialectical Behavior Therapy (DBT): DBT combines standard cognitive-behavioral techniques with mindfulness and acceptance strategies to address intense emotions and improve interpersonal relationships. It is particularly effective for individuals with co-occurring disorders, such as anxiety and borderline personality disorder. Research from the National Institute of Mental Health (NIMH) shows that DBT significantly reduces self-harming behaviors and substance use in patients with emotional dysregulation.
- Individual Therapy: Individual therapy offers one-on-one counseling between the patient and a licensed therapist to address personal issues related to mental health. This therapy allows for deeper exploration of the root causes of mental health disorders, such as trauma, and provides tailored solutions for each individual. A study by the Substance Abuse and Mental Health Services Administration (SAMHSA) found that individual therapy is crucial for recovery, with 70% of patients experiencing improvement in mental health and sobriety.
- Group Therapy: Group therapy involves patients participating in therapy sessions with others who are facing similar challenges. It promotes shared experiences, peer support, and learning through group discussions, making recovery more relatable and less isolating.
- Motivational Interviewing (MI): Motivational Interviewing is a counseling approach that helps individuals explore and resolve ambivalence toward recovery. It encourages patients to voice their reasons for change and strengthens their commitment to treatment. According to the National Institute on Alcohol Abuse and Alcoholism (NIAAA), MI has shown effectiveness in improving treatment retention rates by 25-30%.
- Family Therapy: Family therapy focuses on improving communication, resolving conflicts, and strengthening family dynamics to support recovery. It addresses how family members can contribute to the healing process and develop healthy coping mechanisms.
What Does Triwest Not Cover?
TriWest does not cover certain healthcare services, which include elective procedures, cosmetic surgeries, and services that are deemed medically unnecessary by the Department of Veterans Affairs (VA).
Additionally, it does not cover long-term residential care for non-addictive conditions, experimental treatments, or alternative therapies such as acupuncture and certain herbal medications unless specifically approved by the VA.
TriWest also does not cover services for conditions not related to military service or conditions that are considered pre-existing under their health plans, as well as dental care and vision services, unless they are linked to a broader health issue covered by VA benefits. These exclusions are based on the terms outlined in TriWest’s coordination with VA policies and the specific health needs of veterans.
What Are the Eligibility Criteria for Joining Triwest?
The eligibility criteria for joining TriWest include veterans, active duty service members, National Guard and reserves, family members of eligible veterans and active duty service members, and dependents with special needs. Eligibility is also based on the VA benefits and TRICARE guidelines. Individuals must meet specific requirements to qualify for coverage, ensuring they receive the appropriate healthcare services.
The eligibility criteria for joining Triwest are explained below:
- Veterans: Veterans who are enrolled in the VA healthcare system are eligible for TriWest coverage. This includes veterans with service-connected disabilities or those who have served in active military duty for a specific period, 24 months or more, and are eligible for VA benefits.
- Active Duty Service Members: Active duty service members and their families are eligible for TriWest under the TRICARE program. This includes those serving in the U.S. Army, Navy, Air Force, Marine Corps, and their dependents.
- National Guard and Reserves: Members of the National Guard and Reserves, along with their families, qualify for TriWest coverage when activated or on active duty orders. This provides access to healthcare services similar to those offered to active-duty personnel.
- Family Members of Eligible Veterans and Active Duty Service Members: TriWest covers family members, including spouses, children, and dependents of veterans and active-duty service members. Eligibility for family coverage is based on the sponsor’s active duty or veteran status.
- Certain Dependents with Special Needs: TriWest also covers dependents with special needs, provided they meet the specific criteria set by the VA. This includes children and spouses with conditions such as chronic illnesses or disabilities that require ongoing care.
Contact us today to schedule an initial assessment or to learn more about our services. Whether you are seeking intensive outpatient care or simply need guidance on your mental health journey, we are here to help.
What Are the Benefits of Triwest?
The benefits of TriWest include access to a wide network of healthcare providers, ensuring that veterans and their families have various options for care. Additionally, TriWest offers specialized support for veterans, providing tailored healthcare services that address their unique needs and challenges.
Common benefits of TriWest insurance coverage include:
- Access to a Wide Network: TriWest provides access to a large network of healthcare providers, including specialists, hospitals, and clinics. This wide network ensures veterans can receive care near their homes or wherever they live, reducing the need for long travel. According to a report by the Veterans Health Administration, over 98% of veterans using TriWest have access to a healthcare provider within 30 miles of their home.
- Specialized Support for Veterans: TriWest offers specialized services that are tailored to the unique needs of veterans, such as mental health counseling, dual diagnosis treatment, and military-related health concerns. This support includes services like post-traumatic stress disorder (PTSD) therapy and rehabilitation for physical injuries related to military service. A study by the National Institute of Mental Health found that veterans who receive specialized care are 30% more likely to maintain long-term recovery from mental health disorders.
- Comprehensive Coverage: TriWest offers a comprehensive range of healthcare services, including preventive care, medical treatments, and mental health services.. It ensures that veterans and their families receive all-around care, addressing both physical and mental health needs. According to a study by the National Institute for Health Care Management, comprehensive coverage improves health outcomes by 35% when veterans have access to a variety of treatment options.
- Convenient Referrals: TriWest facilitates convenient referrals to specialist care providers, ensuring that veterans receive timely treatment without unnecessary delays. This streamlined referral system eliminates the need for complex paperwork or waiting for approval, providing faster access to needed services. A 2021 report by the Department of Veterans Affairs found that timely referrals through TriWest reduce wait times for specialty care by up to 40%.
- Affordable Healthcare: TriWest helps reduce the cost of healthcare services for veterans and their families by covering a significant portion of medical expenses. This includes no-cost or low-cost co-pays for many services, making healthcare more accessible. According to a 2022 report by the National Association of Veterans’ Advocates, veterans who use TriWest report a 60% decrease in out-of-pocket healthcare costs compared to non-VA services.
- Access to Emergency Care: TriWest ensures that veterans can access emergency care in times of need, even if they are far from VA facilities. In emergencies, veterans can visit non-VA hospitals, and TriWest will cover the associated costs. According to the Veterans Health Administration, emergency care coverage improves recovery outcomes by providing immediate access to life-saving treatments.
What Are the Alternatives to Triwest?
The alternatives to TriWest include TRICARE, the Veterans Affairs (VA) Health Care System, and private health insurance plans. TRICARE offers comprehensive coverage for active-duty service members, retirees, and their families, with various plans such as TRICARE Prime, TRICARE Select, and TRICARE for Life, each providing different levels of care and coverage.
The VA Health Care System provides veterans with medical care through VA facilities, offering specialized services like mental health support, primary care, and treatment, though it may involve longer wait times and fewer provider options than TriWest.
Private Health Insurance options, such as those offered by employers or through the Affordable Care Act, can serve as alternatives for veterans and their families who do not qualify for TRICARE or VA care, though they come with higher premiums and limited benefits for veterans’ specific needs.
These alternatives offer varying levels of care, cost structures, and access to specialists, allowing veterans and their families to choose the best fit based on their needs and eligibility.
Is TriWest the Same as Tricare?
No, TriWest is not the same as TRICARE, although both are healthcare programs designed for military families and veterans. TriWest is a private company that administers TRICARE benefits through a partnership with the Department of Veterans Affairs (VA), primarily focusing on delivering care through community-based providers.
TRICARE, on the other hand, is the overarching health insurance program for military service members, retirees, and their families, managed by the Department of Defense (DoD). The main difference lies in their scope:
TriWest specifically coordinates care for veterans and their families who are eligible for VA healthcare services, while TRICARE provides a wider range of coverage for active-duty service members, their dependents, and retirees.
TriWest operates under the TRICARE umbrella, but its role is more focused on ensuring that eligible veterans receive healthcare through civilian providers when VA facilities are unavailable or unable to meet their needs.
What Areas Does Triwest Cover in The U.S.?

TriWest covers the following areas in the U.S.:
- American Samoa
- Arizona
- California
- Colorado
- Guam
- Hawaii
- Idaho
- Montana
- New Mexico
- Nevada
- Northern Mariana Islands
- Oregon
- Texas
- Utah
- Washington
- Wyoming
- Alaska
Is Triwest Available in Los Angeles?
Yes, TriWest is available in Los Angeles. Veterans and eligible beneficiaries in the Los Angeles area have access to a network of healthcare providers and services through TriWest, which partners with local healthcare facilities to ensure timely care for veterans.
TriWest offers coverage for various medical, mental health treatments in the region, providing a convenient option for those who may not have access to VA facilities nearby.
LAOP is an approved provider for Blue Shield of California and Magellan, while also accepting many other major insurance carriers.
Check Coverage Now!How to Verify TriWest Insurance in Los Angeles?
To verify TriWest insurance in Los Angeles, you can start by contacting the healthcare provider or facility where you plan to receive services. They typically have a dedicated team to assist with insurance inquiries and can guide you through the verification process.
For insurance verification, you will need to provide your policy information, including your policy number and personal details. This information helps the provider confirm your coverage and determine the services that are included under your plan. It’s advisable to have your identification and any relevant documents ready to expedite the process.
Share This Post














